Grainbach — At the time, bipolar was the diagnosis — but it later became clear it didn’t fully explain what was happening.
What happened to me was something else.
In August, from my internal experience, I wasn’t “cycling.” I wasn’t unraveling. I wasn’t losing myself.
I was over-leveraged.
My brain was pushed into what Californians like to call rocket mode—too much thrust, too little gravity. Venlafaxine flipped a switch in a mind already carrying decades of compressed history: philosophy, literature, religion, trauma, migration, media theory, mythology, and the strange jazz of a world that refuses to stay in one dimension.
What came out didn’t feel like madness to me. It felt like too much data arriving all at once.
I speak in layers because I was born in layers. Damascus will do that to you.
Not just the city, but what it carries: Semitic memory, Greek and Roman ghosts, Christian love, Islamic law, Ottoman bureaucracy, French colonial leftovers, Cold War nationalism, Baathist secularism, and a modern internet that shattered the last illusions of stability.
Add to that a BA in English Literature and an MA in American Cultural Studies, with a specialization in media discourse, networks, globalization—and then place all of it inside a German mental-health system built to operate through clean, linear, two-dimensional categories—effective for standard presentations, but strained when faced with layered, cross-cultural complexity.
I wasn’t ill in a way that could be parsed quickly.
The doctors were worried. They were overwhelmed. They simplified me.
Bipolar became the container—not because it fit perfectly, but because it was safe, recognizable, and administratively manageable.
This is not a story about villains.
It’s a story about overload.
Where it actually began
It began in November 2024.
That’s when suicidal ideation returned—not for the first time in my life. I had known it before: as a child, as a teenager, later as a young man in Jordan during the Syrian war. I knew its voice. I also knew its danger.
Years earlier, I had confessed those thoughts to my best man, André. Another friend, Ioana, once talked me back from the edge. André didn’t make it. He died by suicide in 2019. The wound he left in me became my brakes.
So when those thoughts resurfaced in November 2024, I didn’t romanticize them.
I asked for help.
My Baghdadian house doctor listened. She didn’t rush me. She sat with me, asked careful questions, and made it safe for me to speak honestly. She made call after call until she found a clinic not far from Hof willing to take me. That decision likely saved my life.
A month later, something else happened: the Assad regime began to crumble.
I had feared that moment for years. Assad carried with him the entire post-Ottoman Syrian national project—the secular state that raised me, educated me, and gave me a pluralistic society. It had been dying slowly, painfully. When it finally cracked, something in me loosened.
For the first time, I could let go of a homeland that had refused to die while destroying itself.
I was free to grieve. And to move on.
Clinic, routine, and repair
The clinic helped me more than I can easily say.
The hospital gave me time, routine, healthy food, walking, and reflection. A psychologist suggested what I had long avoided admitting: I needed a different environment, a different pace of life.
The health system granted me extended sick leave. That mattered. It gave me space to heal without immediate economic terror.
A psychiatrist prescribed mirtazapine. It softened the anxiety, slowed my nervous system, and helped me sleep.
And then there was writing. And AI.
Using language—polishing it, questioning it, reflecting it back—I was able to do something close to psychotherapy through text. I grieved my past self. I grieved Syria. I grieved the decade I lost to depression. By early August 2025, I had resolved most of my old traumas.
I was tired. Low-energy. But peaceful.
I was ready to face the present.
The lever that was too strong
On August 9, venlafaxine was added.
Then, unexpectedly, a message arrived from someone who had known me a decade earlier. It reminded me of who I was when I first arrived in Europe—curious, expansive, cosmically oriented, alive.
She had always had a way of disarming me. Not by understanding everything, but by seeing enough to loosen my grip on myself.
The medication activated my mind.
The memory activated my heart.
Together, they sent me into overdrive.
I wasn’t being reckless. I was free. I wanted life.
But my system was suddenly running without limits.
I overreached. I spoke too openly. I tried to integrate too much, too fast.
The people closest to me worried—my wife, my closest friend Stephan. Out of care, they called emergency services.
I didn’t resist. I trusted them. I walked into the ambulance willingly, believing I would be cared for.
What followed was… complicated.
Containment
The encounter at the hospital that night felt procedural rather than human.
Exhausted, I stopped maintaining performative coherence altogether.
That moment was recorded as pathology.
The next day, older psychiatrists convinced me to stay. I didn’t feel I needed hospitalization anymore—my clarity had returned once the venlafaxine stopped—but I trusted them. I shook hands with my doctor. I agreed to follow the plan.
They feared I might hurt myself. Or someone else. They feared escalation.
In that atmosphere, fear became the governing logic.
So they reached for what they knew: antipsychotics.
Observation without medication wasn’t pursued.
The German public health system was under significant pressure. It struggled to hold a mind shaped by layered histories, symbolic thinking, and cross-cultural meaning-making—something that exceeded its available bandwidth at that moment.
Aripiprazole followed. Then more of it.
What came next was not depression. Not mania.
It was neurological agony—akathisia, inner restlessness, emotional flattening, a body screaming to escape itself.
I didn’t want to die.
I wanted the pain to stop.
I learned the system while trapped inside it. With half a mind and a shattered body, I negotiated reductions, insisted on tapering, and eventually left the hospital.
During that period, I was not entirely alone. I was in daily contact with my cousin Roba, based in London, who provided steady, real-time support. Through regular messages, she helped me reflect, asked careful questions, and monitored my condition from a distance at moments when access to my treating psychiatrist was limited.
Roba trained as a general practitioner and worked in a hospital early in her career, before moving through education, arts and culture, and later returning to university to study law—a profession she has practiced for nearly two decades.
Her combined medical and legal literacy proved invaluable. She helped me understand not only the physiological effects I was experiencing, but also the institutional and legal framework I was navigating—allowing me to advocate for myself calmly, avoid unnecessary escalation, and leave care without conflict.
The court declined to mandate continued hospitalization. I was assessed as cooperative and not presenting an immediate risk.
The doctors discharged me with warnings and a warm handshake.
Withdrawal, integration, baseline
I stopped antipsychotics on October 1.
What followed were two difficult months: withdrawal, emotional swings, exhaustion, unpredictability. At the time, I believed I might be dealing with Bipolar II. When I raised that possibility, my psychiatrist rejected the distinction altogether, telling me there was no practical difference between Bipolar I and Bipolar II.
He was unequivocal: without returning to aripiprazole, he said, I would not stabilize. He also made it clear that he was unwilling to continue seeing me unless I agreed to resume antipsychotic medication.
That position didn’t sit right with me. After careful consideration, I declined and chose to continue without antipsychotics, focusing instead on observation, recovery, and stabilization.
I want to be clear about this: I don’t doubt his intentions. He is an older clinician with a good heart, working under heavy load, responsible for more patients than any one person can reasonably carry. Within the limits of his training and context, he acted in what he believed was my best interest.
Where we ultimately diverged was not in care, but in expectation. He asked for a level of trust that exceeded what his framework could reasonably provide—particularly as complexity, language, and perspective began to matter. I trusted him as far as that framework allowed, and no further.
He did, however, offer a further four weeks of sick leave. When that period ended, I was noticeably more stable—sleeping, thinking clearly again—but still exhausted, not yet fully myself.
Not wanting to burden him further, I returned to my Baghdadian general practitioner, who reassessed my condition and extended my sick leave until I was genuinely ready to re-enter the world.
Two practices helped me stabilize during this period: reading reflective writing on suffering, and keeping a disciplined daily journal—tracking my recovery, questioning my assumptions, and actively challenging my own thinking.
My fluency in English also mattered. It allowed me to access a broader body of international research and clinical discussion on mood disorders, including the ways complex, trauma-driven depression can resemble bipolar presentations. That wider perspective helped me contextualize my experience beyond any single national or institutional frame.
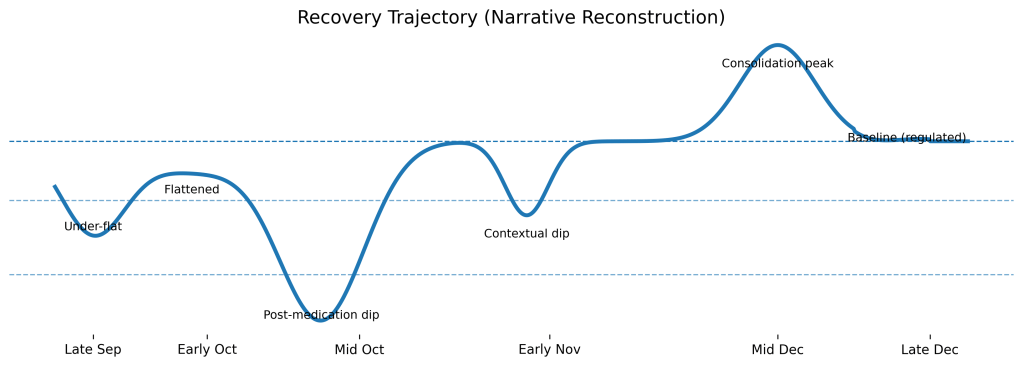
Looking back now, what best explains my experience is long-standing, trauma-driven unipolar depression, complicated by antidepressant-induced hypomania and medication-related injury.
Not a cycle.
A recovery curve.
And now—finally—I’ve reached baseline.
I sleep well. I think clearly. I negotiate conflict without collapsing.
For the first time in ten years, I’m learning German willingly—thirty minutes a day, calmly, without resistance.
That alone tells me everything.
The naked truth
When I came out of depression, I came out naked.
Just as my internal defenses fell away, I exposed my mind and soul to the people closest to me—my wife, my closest friend, and a friend of ten years who felt like a soulmate.
I was Damascus trying to rebuild itself in days after a war that lasted thirty-four years, beginning with a childhood trauma at age four—the same dynamics that later tore Syria apart.
This is my inheritance: destruction, then reconstruction. Again and again.
And here I am, trying to rebuild myself in Central Europe.
There are a million Syrians in Germany alone. Most will return home. A few will stay. Fewer still will try to translate something ancient into this new terrain.
I am one of them.
And yet, I’ve learned the hard way that even one person can be too much.

What scares me now
Over the past ten years, I’ve learned to navigate an academia stalled in discourse, a bureaucracy hostile to mobility, corporations driven by scale, and healthcare systems built for containment rather than enablement in this part of the world—while also living through the collapse of a nation I once called home.
I can deal with machines.
What unsettles me are the people who live inside them.
Societies conditioned by rigid systems demand honesty but fear truth. They enforce boundaries without intimacy, privacy without trust, stability without reflection.
When I decompressed, the first people shocked by my undepressed self were the ones I loved most. Some avoided me. Some tried to manage me. Some reacted with anger.
I won’t pretend that didn’t hurt. It did. But I’ve come to understand that what felt like rejection was often fear—fear of change, fear of losing familiar ground.
If my truth is too much for those closest to me, how can I feel safe in the wider society?
I don’t know the answer yet.
Should I return to Damascus—imperfect, dangerous for minds like mine, but emotionally literate?
Should I move to Ireland—more humane, more relational, more honest, but economically punishing, with a housing crisis that turns belonging into a constant negotiation?
I don’t know.
All I know is this:
Everything is more real now. More demanding. More alive.
And for the first time in decades, I feel equipped to try.
Dedication
This piece exists because I was not alone.
To my steady point of light across a decade, reminding me who I was when my own sense of self faltered.
To André — whose absence remains a quiet weight beneath my life, and whose memory continues to shape how seriously I hold it;
and to Ioana — who once stayed with me at the edge, long enough for me to step back.
To Nizar, Tante Zainab, and Ermanno — who planted the first seeds of love in me, across poetry, kinship, and quiet hospitality, and taught me to follow love itself before any doctrine.
To Deniz and Manar — who helped keep me safe and sane through the harsh political climate in Syria, before and after the war.
To Tarek and Mudar — two steady stars of inspiration.
To my father, my mother, and my stepmother — who raised us, and gave me the brightest two brothers I could ever imagine: rock-solid friends and allies — and to Khallo Jalal, Khallo Bassem, and Jeddo Baha’ al-Din, who inspired, cared for, and protected me in my youth.
To Udai, who opened the door to the beauty and freedom of thinking in English, widening both my sense of self and my place in the world.
To Kris and Jake, who welcomed me into the world of journalism.
To Housi and Mones — who helped me find my rhizome, and trust it to grow.
To Sarah — whose endurance, care, and presence carried far more weight than words can measure, especially through years of exile and separation from family.
To Stephan — a father-like friend who guarded me when my own bearings failed, and who stood watch when help was needed most.
To Roba — my god-cousin, whose love, medical judgment, legal clarity, and steady, selfless care helped me navigate moments I could not manage alone.
To Nassem — my cousin, who prepared me early for the fights life would later bring.
To Maria and Melanie, Rudy and Alex, Drew and Liza, Melissa and Fida, Marion and Clara, Senka and Jessica, Inas and Majida, Ahmad and Ali, Ben and Tye, Astrid and Michi, Niko and Chris — readers, witnesses, and friends who made my words feel received rather than sent into the void.
To Gaby and Nancy — true friends and public servants — who offered refuge, access, and a path toward integration.
To Thomas and Father Martin — quiet guardians grounded in love and light.
To Reem — my general practitioner, who extended herself beyond reasonable limits when the health system could not.
And to the clinicians and nursing staff at the psychiatrist clinic — whose care, patience, and humanity mattered deeply, even within imperfect circumstances.
I remain responsible for my recovery.
But I did not recover in isolation.
You were my village lanterns.
Relevant Links
How to Suffer Gracefully
Unappreciated
My Theory of Everything
When Healing Became Another Battle
House of Salted Caramel
Good Things Can Always Wait
Damascus in Vienna

3 thoughts on “Decompressed: Between Damascus and Vienna”